Healthcare fraud investigation typically starts when the enforcement found an attempt to obtain money or other items of value from a healthcare company or government program through false and fraudulent representations.
In most healthcare fraud trails, the intent of the defendant or defendants is a central issue; in other words, the jury is asked to determine whether the accused purposefully sought to fraudulently obtain payment from the healthcare payor.
The government usually relies heavily on errors in billing or coding to demonstrate that defendant’s intent to defraud the healthcare company. However, such errors – even if they are repetitious – clearly do not definitively prove that the defendant intended to defraud the government by making a false claim.
Current estimates indicate that between three and ten percent of total healthcare spending in the U.S. is fraudulent. This represents between approximately $68 billion and $230 billion dollars annually.
Whichever estimate you choose to believe, healthcare fraud is one of the largest financial problems that the country currently faces. This is why many state and federal agencies have been granted extraordinary authority and resources to go after cases of healthcare fraud, specifically Medicare and Medicaid fraud.
This means that virtually every professional within the medical industry has been saddled with onerous compliance burdens, and many have been unjustly targeted by heavy-handed law enforcement operations.
Burden of Proof in a Healthcare Fraud Investigation
To prevail in a healthcare fraud investigation, the government must prove that the defendant knowingly participated in a scheme to defraud either a federal healthcare program (DOL, Tricare, Medicaid, Medicare), a state or local healthcare program, or a private insurer. For criminal trials, the burden of proof is beyond a reasonable doubt. In civil trials, the burden of proof is a preponderance of the evidence.
Common Examples
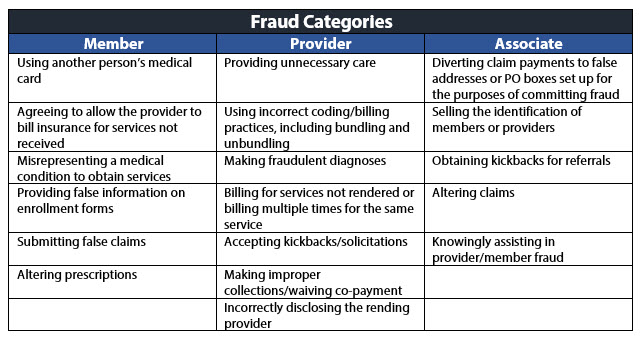
Healthcare fraud encompasses a wide variety of conduct; the common thread is that the actions at issue were carried out for the purpose of illegally obtaining a benefit for a healthcare provider at the expense of the state or federal government or private insurer. Below is a non-exclusive list of the types of cases the government commonly prosecutes:
- Fraudulent certification occurs when a person fraudulently signs or forges a required certification, such as a certification that services were actually provided or were medically necessary. Healthcare payors often require several such certifications from healthcare providers.
- Upcoding occurs when a provider submits a claim for a procedure or service that is paid at a higher rate than the procedure or service actually performed.
- Unbundling is another method of gaming the billing codes, in which the healthcare provider separates out procedures that are commonly billed as one group in order to obtain additional payments for each part of the group procedure.
- Services not rendered, or “phantom billing”, occurs when a healthcare provider submits a bill for a procedure or service that was never performed.
- Imaginary patients or “ghost patients” are patients for whom a provider falsely claims to have performed services or procedures to or persons who were never seen by the provider.
- Lack of medical necessity is charged when the government alleges that, despite receiving the proper certification, the services rendered to the patient were not medically necessary.
- Kickbacks are one of the biggest areas of healthcare fraud and involve providing compensation in exchange for referrals. It is illegal to pay for any referral of a government healthcare patient in any manner, whether monetarily or through gifts. Both the person offering the payment and the person receiving the payment may be charged for participating in a kickback scheme.
- The Stark Law prevents physicians from maintaining a financial interest in services to which they refer their patients, such as toxicology labs and pharmacies. There are several safe harbor exceptions to the Stark Law that must be closely followed to comply with the law.
Penalties
Our ultimate goal at Heath Hyde in all of our healthcare fraud representation is to avoid criminal investigations. Whether civil or criminal, healthcare fraud penalties can be extremely severe and include recoupment requests, non-payment of future claims, civil fines of up to $ 11,000 per false claim, exclusion from federal healthcare programs, treble damages, attorney fees, criminal fines, criminal indictment, or imprisonment. We often succeed in keeping such investigations on the civil path, protecting our clients’ medical licenses and freedom.
Defending Healthcare Fraud

At Heath Hyde, our team of former healthcare prosecutors and experienced defense attorneys have a distinguished history of protecting individual providers, hospitals, laboratories, pharmacies, home healthcare entities, and many other healthcare business owners against charges of healthcare fraud, whether civil or criminal in nature. In most instances, such investigations have resulted in a formal statement by the government that our client had no civil or criminal liability. Recent examples include:
- Medicare Fraud
- False Claims Act Violations
- Tricare Fraud
- Stark Law Investigations
- Anti-Kickback Investigations
- Medicare Audit
- Department of Labor Investigations
- FBI, DEA, FDA, and Medical Board Investigations
- OIG Subpoenas
- Grand Jury Subpoenas
Heath Hyde Is the Defense Team You Need To Have on Your Side
If you have been charged with a healthcare-related violation, are currently under investigation by civilian or law-enforcement agencies, or believe that you may be under investigation, Heath Hyde can help you resolve the issue without the catastrophic consequences that often result.
Our law firm is made up of lawyers who have worked on both sides of the courtroom, as experienced defense attorneys and prosecutors at both the state and federal levels. Our lawyers bring formidable experience and knowledge that is specific to the highly complex field of healthcare law.
If you believe that you or your practice may be under investigation by the Office of the Inspector General, the FBI, the Department of Justice, the Centers for Medicare and Medicaid Services, or any other agency, the first thing that you should do is call Heath Hyde as soon as possible. We can help you navigate through the early stages of a criminal or civil case. The mere fact that prosecutors are aware that the party under investigation has retained experienced legal counsel with a strong track record of winning is enough to convince them to abandon criminal charges.
Even if you are charged, sued, or have administrative action taken against you by an agency, we can help minimize the fallout. This includes helping you avoid career-stopping administrative actions such as license revocation or fines.
If You Believe You or Your Practice Is Under Investigation, Call a Lawyer Now
In addition to being very complex, U.S. healthcare law typically carries draconian penalties for violators. This is a result of the enormous threat that healthcare fraud, especially where the government itself is the victim, poses to the country. As the fiscal situation within America’s healthcare situation continues to worsen, politicians, law enforcement, and civilian administrators are looking to make examples of those who they perceive to be driving medical costs ever higher.
This means that investigators, auditors, compliance agents, and law enforcement have been afforded nearly unlimited resources to track down and implicate those who violate the country’s healthcare laws, particularly those involving fraud. However, this zeal to secure convictions has led to the casting of a wide net in which many innocent parties are entangled each year. In fact, most investigations begin due to innocent error, negligence, or incompetence on the part of healthcare providers.
Unfortunately, ignorance of the law is no excuse. Many healthcare statutes are written in a way that allows for conviction of serious crimes even when no outright criminal intent has been established. Some laws allow for criminal conviction when it can be shown that the defendant did no more than willfully ignore protocols.
This all means that if you even think that you may be under investigation, you need to call Heath Hyde or another similarly experienced and proven legal team to get in your corner early in the fight. This is when you have the most leverage against investigators who are building a case.
Recognizing When You May Be Under Investigation

In some instances, law enforcement may be very careful not to alert you to the fact that your practice is currently being investigated for Medicare or other healthcare fraud. However, most of the time, you will have clear warning signs.
Do not ignore these. If you have substantial reason to believe that you, your practice, or any of your employees may be under investigation, call an experienced lawyer today. As healthcare fraud lawyers, the earlier we get involved in a case, the greater the chance that we will be able to steer towards a desirable outcome.
You should immediately contact an attorney if you notice any of the following activities:
- Any current or former patient lets you or your office know that they have been contacted by law enforcement regarding their relationship with you.
- You are contacted by any administrative official or law enforcement agent, even if the encounter appears casual.
- Receiving a subpoena.
- Receiving a letter from any U.S. attorney indicating that you or your practice may be the target of an investigation.
- You are questioned in any way by someone identifying themselves as a government agent.
- Receiving a letter requiring any action that stems from a Medicare False Claims Act case.
- Any colleagues, employees, or even competitors being arrested, detained, interrogated, or investigated. Even if you have no direct business relationship with another practice that is under investigation in your field, this can still be a strong indicator that you may be next.
- The freezing of any business or personal bank accounts by authorities.
- Search warrants being executed at your practice.
You should understand that federal agencies do not passively investigate; if agents are investigating you, they believe strongly that they will find something that will stick in court. You need to get an experienced legal team that has extensive expertise in healthcare fraud cases on your side before it’s too late.
You Almost Can’t Do Business Without Potentially Violating Some Law
If you operate a medical practice or are a medical professional working within a medical practice that provides designated health services to Medicare or Medicaid patients, you would need to be almost superhuman to avoid running afoul of the myriad of statutes that regulate your every move.
Heath Hyde has decades of experience handling the six main statutory categories under which all providers of healthcare services operate. These are:
- The False Claims Act, also known as the Lincoln Law. This is the main statue dealing with cases where the government has been defrauded.
- Stark Laws. These are a set of laws prohibiting physician self-referral. While there are exceptions, it is generally illegal for medical professionals to refer to Medicare or Medicaid patients to family members or practices in which the physician or family has a financial interest.
- The Anti-Kickback Statute. Federal law prohibits any remuneration for referrals of patients that are part of the Medicare or Medicaid systems.
- Prescription fraud laws. Not properly following prescription guidelines is often a criminal violation that is defined as a felony. With the opioid crisis ravaging the nation, law enforcement is turning up the heat on so-called pill mills.
- Bribery laws. Medical professionals generally cannot accept remuneration that may affect medical decisions of any kind. This is particularly true in the case of pharmaceutical companies offering perks, monetary or otherwise, to physicians who their drugs.
Each one of these areas of legal practice is byzantine. The complex case law that has sprung up around them often defies common sense. Many people are convicted of Medicare fraud and need an attorney for actions that most people would easily recognize as being fraudulent, such as intentionally billing for a procedure or service that was never rendered.
However, other cases where individuals have been investigated, charged, and convicted aren’t nearly so black and white. Consider all of the different ways in which people are frequently convicted, fined, and sent to prison for Medicare fraud:
- Overutilization of equipment, services, or procedures. This is an area that will always be gray. Where exactly should the line be drawn when determining whether a physician was acting according to the maxim better safe than sorry, or simply trying to pad their own pockets? At Heath Hyde, we have the extensive case law knowledge to draw those lines and keep our clients on the right side of the law.
- Submitting false claims. When outright false claims are submitted, it may seem like an open-and-shut case. However, in order for the charges to stick, there can be no room for doubt that the defendant submitted the claim knowingly or willfully. Our lawyers are adept at raising that doubt.
- Billing for drugs, services, or products that were never actually provided. Honest mistakes happen. Our law firm knows the relevant statutes inside and out. We’ll always ensure that our clients are not railroaded if their actions don’t meet the criteria for establishing the criminal intent that is a predicate to actual fraud.
- Ghost patients. Although submitting claims for patients that don’t exist or are not actual patients of the practice can be a crime, there are many reasons why such accusations may not legally prevail in court.
- Billing for medically unnecessary goods or services. The definition of medically unnecessary is highly context specific and is almost never clear cut. Our lawyers have successfully challenged assertions of medically unnecessary treatment throughout each phase of the legal process.
- Unbundling. If an ICD-10 procedure code includes multiple services, using the service-specific code again for any of those services individually constitutes unbundling, which is a crime.
- Up-coding. This is billing for a higher-cost code than the service actually rendered.
This is just a cross-section of the instances in which people have been convicted, fined, and imprisoned for healthcare fraud. However, all of the above-listed activities may also be innocent mistakes under certain circumstances. The trick is to raise as much doubt as possible that there was any real criminal intent. Even at the investigation stage, most agencies do not want to waste manpower and resources on cases that are unlikely to result in some kind of conviction or major civil infraction. Heath Hyde will raise the issues that make those agencies take a second look at their chances of prevailing.
Those who are eventually charged with crimes stemming from a healthcare fraud investigation are frequently hit with charges that are not specific to Medicare or healthcare fraud. Our legal team has decades of experience fighting these charges, which can include:
- Money laundering. This occurs when there is any actual hiding or attempt to hide the origin of illicit proceeds.
- Attempt or conspiracy to commit healthcare fraud. If someone participates in an act of healthcare fraud, even if they play only a minor part or don’t directly benefit from it, they are still technically guilty of conspiracy. Likewise, if healthcare fraud was attempted but unsuccessful, the attempting party can still be convicted of the crime as if it had been successfully carried out.
- Wire fraud. Any monetary crime that involves the use of interstate communications technologies also opens the defendant up to charges of wire fraud. Many federal cases are disposed of after the defendant pleads guilty to a single count of wire fraud. However, the maximum sentence on a single count is 30 years.
Each one of these charges is serious, potentially carrying decades in prison. Heath Hyde has extensive experience in defending against them.
The Consequences of an Investigation Into Healthcare Fraud Can Be Devastating

Spending 50 years in prison, such as the sentence that was recently handed down to a Florida doctor who was convicted of Medicare fraud, would be a horrible way to live out your final decades. In 2017, 639 people were convicted of health care fraud in the United States. Most of them served some prison or jail time. Many are still incarcerated.
Yet this represents just a fraction of the total investigations that take place each year. The FBI and Department of Justice alone investigate thousands of such cases annually. Many of these will end not in criminal convictions, but in civil or administrative actions against the alleged perpetrators.
Even if you believe that you won’t be criminally convicted as the result of a healthcare fraud investigation, you need to approach the potential civil and administrative consequences with equal seriousness.
It’s true that the most life-altering sanctions that may arise from a healthcare fraud investigation are those involving jail or prison time. In cases of healthcare fraud, a defendant who is convicted may be sentenced to as many as ten years in prison. If bodily injury or death has occurred as a result of the commission of the fraud, that penalty may raise to 20 years. Furthermore, someone who has merely conspired to commit the fraud, even if they have not directly benefited from it, may be sentenced to up to 20 years in cases where bodily injury or death have resulted.
For those who have made false claims within the Medicare system, each count can carry up to five years in prison. For repeat offenders, a sentence of up to life in prison may be imposed.
In cases that involve wire fraud, which technically occur in a large number of healthcare fraud cases due to the near inevitability of using a computer, phone, or other communications device, a convicted defendant may be sentenced to up to 30 years in prison.
Non-Prison Penalties

As bad as the prospect of spending decades behind bars may be, the non-prison penalties for healthcare fraud can also be severe.
For anyone who is found to have violated the False Claims Act, up to $21,000 in fines for each act may be assessed. Additionally, restitution of up to three times the amount that the government was defrauded may be imposed. If it is determined that the violation was committed with full knowledge and criminal intent, then a fine of up to $250,000 may be imposed.
Similarly, any violation of the Anti-Kickback Law may result in a fine of up to $50,000 per instance, as well as the imposition of damages equal to as much as three times the loss to the government. Someone found guilty of health care fraud can be assessed a fine of up to $250,000.
Other problems can arise from administrative and other civil actions that may be taken against the subject of a healthcare fraud case. Such individuals may face the suspension or outright revocation of their medical licenses. This is usually a career-ending situation.
Medical professionals may also lose their DEA registration, preventing them from prescribing medictions and, in many cases, making practicing their specialty difficult or impossible. Payment of current outstanding Medicare or Medicaid invoices may be permanently withheld, or medical personnel may be completely excluded from participation in any government healthcare programs. Medical staff may also face immediate termination by their employers even if no criminal conviction results from an investigation.
CHOOSING THE RIGHT DEFENSE Team
In some cases, an ability to demonstrate that the defendant had no knowledge or intent to defraud will be enough to convince the government to reach a speedy and favorable resolution. However, that is not always the case.
For example, in cases where unnecessary services were rendered, the determination of guilt or innocence may come down to the standard of care that was provided. In such cases, our in-depth knowledge of relevant Diagnosis Related Groups, Clinical Practice Guidelines, and Current Procedural Terminologies enable us to provide the optimum defense. Handling these situations as criminal matters may be completely inappropriate, but that is how the government chooses to handle a large number of such cases. Heath Hyde can help defend you and your practice from specious charges stemming from mistakes or deviations from standard clinical protocols.
HEATH HYDE Is Very Effective IN NEGOTIATIONS WITH GOVERNMENT agents
While the goal should always be to resolve cases as quickly and painlessly as possible, Heath Hyde believes that a full willingness to take a case all the way through the trial process is a necessary component to providing the best possible defense for our clients.
With a long track record of winning at trial, showing up at a hearing or interview with a Healthcare Fraud Group attorney will clearly signal to investigators or prosecutors that our client means business. The last thing that government agencies want to do is waste tens or hundreds of thousands of dollars taking a case to trial when there is a significant possibility that they will lose.
This is when the complexity of healthcare fraud statutes can become an asset. Heath Hyde welcomes taking clients’ cases to trial because the cases often defy common sense. Juries are unlikely to sympathize with highly abstract or arcane legal theories. Heath Hyde is comprised of skilled trial lawyers who use their rhetorical facility and ironclad arguments to win over juries, even where the legal technicalities may favor the prosecution.
This courtroom wildcard gives us a powerful bargaining chip at early stages of the negotiations, ensuring that even when the charges are not dropped outright our client and the government can reach a workable agreement.
HEATH HYDE PUTS FORMIDABLE ALLIES ON YOUR SIDE
Heath Hyde has been handling healthcare and Medicare-related cases for decades.
We have a network of industry-leading team members across the country. Many of our lawyers have experience working in the same government agencies against which they are now fighting on behalf of our clients. From former U.S. Attorneys to ex-Department of Justice lawyers, our team members have a breadth and depth of experience that few others can bring to the table.
If you are the target of a healthcare fraud investigation or have been charged with a healthcare-related crime, contact Heath Hyde today by calling or visiting our website. Let our expert lawyers go to work for you and maximize the chance of a satisfactory outcome of your case.
Heath Hyde has:
- Won OVER 90% of TRIALS AND ARBITRATIONS.
- We travel across the country to meet with you.
- We feel an obligation to correct wrongs in the fraud community.
- 400+ Trials & Arbitrations.
- $100s of Millions in Savings to Defendants.
- 1,000s of Dismissals, Acquittals & Declinations of Prosecutions

Our healthcare fraud defense attorneys assist service providers and businesses under investigation for alleged Qui Tam Lawsuit, Stark Law, False Claims Act, or Anti-Kickback violations. We are available every day of the year, 24 hours a day. You can call us directly or complete our contact form for a confidential case analysis & review.
AVOID A HEALTHCARE FRAUD INVESTIGATION, CALL HEATH HYDE
Call 903.439.0000 Including Weekends.